About the Journal
Scope of the Journal
Indexed In
Journal Information
Current issue
Archive
Editorial Board
Journal Policy
APC Policy
Authorship Policy
Author Recognition Policy
Citation Policy
Conflict of Interest (COI) Policy
Copyright Policy
Data Availability Policy
DEI Policy
Digital Archiving Policy
Ethical Approval Policy
Funding Policy
Image Policy
Open Access Policy
Ownership & Governance
Peer Review Policy
Personal Data Protection Policy
Plagiarism Policy
Post-Publication Policy
Preprint Policy
Author Instructions
Submit Manuscript
Contact Information
Journal Policy
APC Policy
Authorship Policy
Author Recognition Policy
Citation Policy
Conflict of Interest (COI) Policy
Copyright Policy
Data Availability Policy
DEI Policy
Digital Archiving Policy
Ethical Approval Policy
Funding Policy
Image Policy
Open Access Policy
Ownership & Governance
Peer Review Policy
Personal Data Protection Policy
Plagiarism Policy
Post-Publication Policy
Preprint Policy
RESEARCH PAPER
Antibacterial activity of Moringa oleifera, Solanum nigrum, and Sesbania grandiflora against Bacteria isolated from wound infections
1
PG & Research Department of Biotechnology and Bioinformatics, Holy Cross College (Autonomous), Affiliated to Bharathidasan University, Tiruchirappalli, India.
2
Department of Microbiology, K.A.P Viswanatham Govt Medical College, Tiruchirappalli, India.
Submission date: 2025-09-21
Final revision date: 2025-11-18
Acceptance date: 2025-12-07
Online publication date: 2026-01-28
Publication date: 2026-01-28
Journal of Medico Informatics 2026;02(Issue 01):12-16
HIGHLIGHTS
- Medicinal plant extracts showed antibacterial activity against wound infection bacteria.
- Ethanol extracts exhibited higher antibacterial activity due to phytochemical compounds.
- Solanum nigrum demonstrated strongest antibacterial activity among tested medicinal plants.
- Antibacterial activity increased with extract concentration in agar diffusion assays.
- Plant-derived compounds may serve as alternative antimicrobial agents against resistant bacteria.
KEYWORDS
TOPICS
ABSTRACT
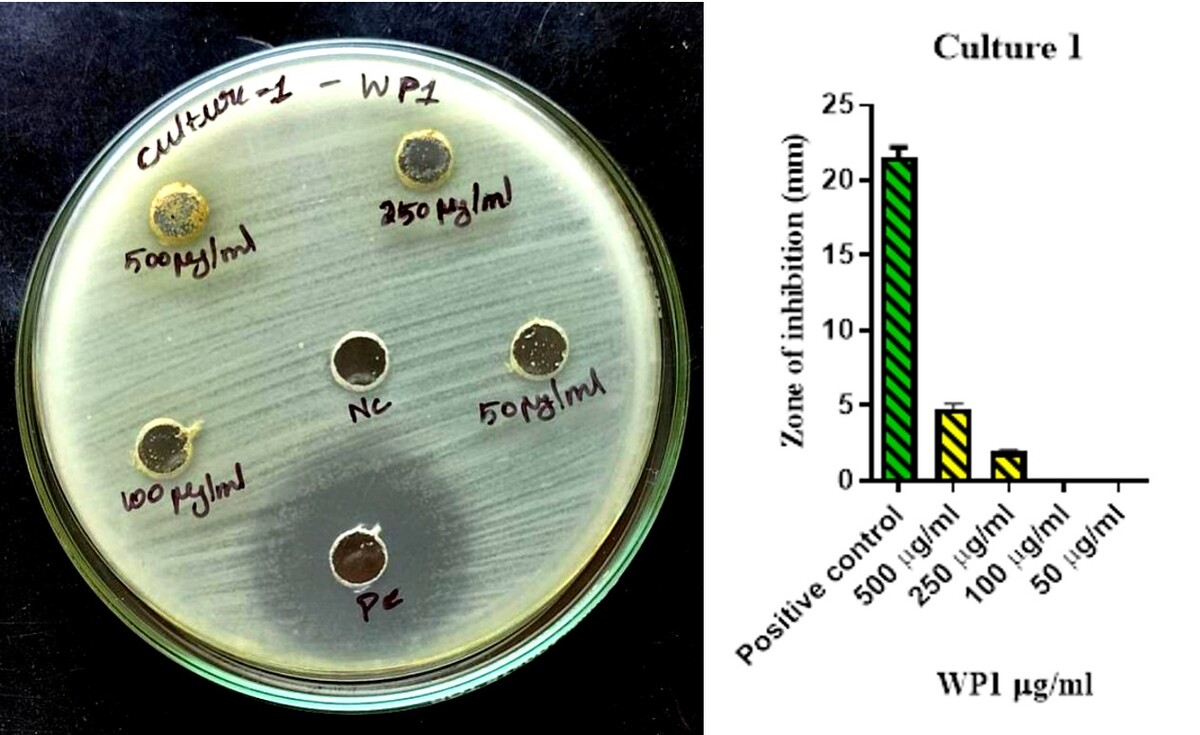
Around the world, most of the medical systems usually employ medicinal herbs to treat both acute and chronic wounds. The current study aims to evaluate the antibacterial properties of Moringa oleifera, Solanum nigrum, and Sesbania grandiflora. These plants were tested for antibacterial activity against wound infections by collecting and extracting the plant’s crude material. By using the Hanging drop method and the agar-well diffusion method, three distinct bacterial colonies were identified. Ethanol extract showed the most significant antibacterial activity, attributed to the presence of alkaloids, tannins, saponins, phenols, and steroids. The antibacterial activity varied for different test samples of 500 µg/ml, with the positive control serving as a reference of the expected effect. Solanum nigrum's potent antibacterial properties suggest its potential as a valuable natural resource in combating bacterial diseases, potentially aiding in future herbal medicine and pharmaceutical research. The results suggest these plants could be valuable natural resources for combating bacterial diseases.
ACKNOWLEDGEMENTS
The authors thankfully acknowledge the Department of Science and Technology, Government of India, for providing support through the Fund for Improvement of S&T Infrastructure in Universities and Higher Educational Institutions (FIST) program (Grant No. SR/FIST/College /2020/943).
FUNDING
Department of Science and Technology, Government of India, through the Fund “Improvement of S&T Infrastructure in Universities and Higher Educational Institutions (FIST) program (Grant No. SR/FIST/College /2020/943)”
CONFLICT OF INTEREST
The authors declare that they have no known financial, personal, academic, or other relationships that could inappropriately influence, or be perceived to influence, the work reported in this manuscript. All authors confirm that there are no competing interests to declare.
PEER REVIEW INFORMATION
Article has been screened for originality
REFERENCES (27)
1.
Abdallah EM, Alhatlani BY, de Paula Menezes R, Martins CHG. (2023), Back to Nature: Medicinal Plants as Promising Sources for Antibacterial Drugs in the Post-Antibiotic Era, Plants (Basel), 12(17) doi:10.3390/plants12173077. PMID: 37687324.
2.
Ademiluyi AO, Aladeselu OH, Oboh G, Boligon AA. (2018), Drying alters the phenolic constituents, antioxidant properties, alpha-amylase, and alpha-glucosidase inhibitory properties of Moringa (Moringa oleifera) leaf, Food Sci Nutr, 6(8):2123-2133. doi:10.1002/fsn3.770. PMID: 30510713.
3.
Asmerom D, Kalay TH, Tafere GG. (2020), Antibacterial and Antifungal Activities of the Leaf Exudate of Aloe megalacantha Baker, Int J Microbiol, 2020:8840857. doi:10.1155/2020/8840857. PMID: 33061982.
4.
Barua CC, Begum SA, Sarma DK, Pathak DC, Borah RS. (2012), Healing efficacy of methanol extract of leaves of Alternanthera brasiliana Kuntze in aged wound model, J Basic Clin Pharm, 3(4):341-5. doi:10.4103/0976-0105.105336. PMID: 24826048.
5.
Bernatchez SF, Bichel J. (2023), The Science of Skin: Measuring Damage and Assessing Risk, Adv Wound Care (New Rochelle), 12(4):187-204. doi:10.1089/wound.2022.0021. PMID: 35904378.
6.
Bibi N, Perveen S, Kanwal S, Latif F, Rashid R, Janiad S, Qadeer I, Naseem F, Alanzi AR, Herqash RN, Haider I, Abbasov MA, Kayani S, Shah MA. (2025), Investigation of Antimicrobial Potential of Medicinal Plants Against Pseudomonas aeruginosa, Food Sci Nutr, 13(11):e70999. doi:10.1002/fsn3.70999. PMID: 41245185.
7.
Chen X, Dai X, Liu Y, Yang Y, Yuan L, He X, Gong G. (2022), Solanum nigrum Linn.: An Insight into Current Research on Traditional Uses, Phytochemistry, and Pharmacology, Front Pharmacol, 13:918071. doi:10.3389/fphar.2022.918071. PMID: 36052142.
8.
Chinemerem Nwobodo D, Ugwu MC, Oliseloke Anie C, Al-Ouqaili MTS, Chinedu Ikem J, Victor Chigozie U, Saki M. (2022), Antibiotic resistance: The challenges and some emerging strategies for tackling a global menace, J Clin Lab Anal, 36(9):e24655. doi:10.1002/jcla.24655. PMID: 35949048.
9.
Cleary T, Miller N, Martinez OV. (2002), Evaluation of wet-prep motility test for presumptive identification of bacillus species, J Clin Microbiol, 40(2):730. doi:10.1128/JCM.40.2.730.2002. PMID: 11826010.
10.
El-Sherbiny GM, Alluqmani AJ, Elsehemy IA, Kalaba MH. (2024), Antibacterial, antioxidant, cytotoxicity, and phytochemical screening of Moringa oleifera leaves, Sci Rep, 14(1):30485. doi:10.1038/s41598-024-80700-y. PMID: 39681592.
11.
Keita K, Darkoh C, Okafor F. (2022), Secondary plant metabolites as potent drug candidates against antimicrobial-resistant pathogens, SN Appl Sci, 4(8):209. doi:10.1007/s42452-022-05084-y. PMID: 35821909.
12.
Kumar A, Sebastian CL, Vinod V, Varghese L, Venugopal A, Biswas L, Gopalakrishna R, Biswas R. (2025), Filamentous forms of Gram-negative bacteria on microscopy: Report of a case and review of literature, Indian J Med Microbiol, 55:100864. doi:10.1016/j.ijmmb.2025.100864. PMID: 40273988.
13.
Lee JE, Jayakody JTM, Kim JI, Jeong JW, Choi KM, Kim TS, Seo C, Azimi I, Hyun JM, Ryu BM. (2024), The Influence of Solvent Choice on the Extraction of Bioactive Compounds from Asteraceae: A Comparative Review, Foods, 13(19) doi:10.3390/foods13193151. PMID: 39410186.
14.
Mogana R, Adhikari A, Tzar MN, Ramliza R, Wiart C. (2020), Antibacterial activities of the extracts, fractions and isolated compounds from Canarium patentinervium Miq. against bacterial clinical isolates, BMC Complement Med Ther, 20(1):55. doi:10.1186/s12906-020-2837-5. PMID: 32059725.
15.
Muteeb G, Rehman MT, Shahwan M, Aatif M. (2023), Origin of Antibiotics and Antibiotic Resistance, and Their Impacts on Drug Development: A Narrative Review, Pharmaceuticals (Basel), 16(11) doi:10.3390/ph16111615. PMID: 38004480.
16.
Nwankwo EO, Nasiru MS. (2011), Antibiotic sensitivity pattern of Staphylococcus aureus from clinical isolates in a tertiary health institution in Kano, Northwestern Nigeria, Pan Afr Med J, 8:4. doi:10.4314/pamj.v8i1.71050. PMID: 22121413.
17.
Ofori-Kwakye K, Kwapong AA, Bayor MT. (2011), Wound healing potential of methanol extract of Spathodea campanulata stem bark formulated into a topical preparation, Afr J Tradit Complement Altern Med, 8(3):218-23. doi:10.4314/ajtcam.v8i3.65280. PMID: 22468000.
18.
Pareek A, Pant M, Gupta MM, Kashania P, Ratan Y, Jain V, Pareek A, Chuturgoon AA. (2023), Moringa oleifera: An Updated Comprehensive Review of Its Pharmacological Activities, Ethnomedicinal, Phytopharmaceutical Formulation, Clinical, Phytochemical, and Toxicological Aspects, Int J Mol Sci, 24(3) doi:10.3390/ijms24032098. PMID: 36768420.
19.
Parker GD, Plymale A, Hager J, Hanley L, Yu XY. (2025), Molecular imaging uncovers growth media influence on biofilms' EPS production, Front Chem, 13:1703055. doi:10.3389/fchem.2025.1703055. PMID: 41756812.
20.
Raghuvanshi D, Dhalaria R, Sharma A, Kumar D, Kumar H, Valis M, Kuca K, Verma R, Puri S. (2021), Ethnomedicinal Plants Traditionally Used for the Treatment of Jaundice (Icterus) in Himachal Pradesh in Western Himalaya-A Review, Plants (Basel), 10(2) doi:10.3390/plants10020232. PMID: 33504029.
21.
Ramsay S, Cowan L, Davidson JM, Nanney L, Schultz G. (2016), Wound samples: moving towards a standardised method of collection and analysis, Int Wound J, 13(5):880-91. doi:10.1111/iwj.12399. PMID: 25581688.
22.
Roointan A, Kamali-Kakhki R, Fathalipour M, Hashemi Z, Zarshenas MM, Soleimani M, Mirjani R. (2020), Antibacterial Activity of Prunus Scoparia Root Methanol Extract against Most Common Burn Wound Pathogens, Iran J Med Sci, 45(6):444-450. doi:10.30476/ijms.2019.82071. PMID: 33281261.
23.
Salam MA, Al-Amin MY, Salam MT, Pawar JS, Akhter N, Rabaan AA, Alqumber MAA. (2023), Antimicrobial Resistance: A Growing Serious Threat for Global Public Health, Healthcare (Basel), 11(13) doi:10.3390/healthcare11131946. PMID: 37444780.
24.
Shokryazdan P, Sieo CC, Kalavathy R, Liang JB, Alitheen NB, Faseleh Jahromi M, Ho YW. (2014), Probiotic potential of Lactobacillus strains with antimicrobial activity against some human pathogenic strains, Biomed Res Int, 2014:927268. doi:10.1155/2014/927268. PMID: 25105147.
25.
To SW, Sani MH, Malek N, Susanto H, Endharti AT, Permatasari HK, Zhang T. (2026), Phytochemical Analysis of Different Plant Organs of Bauhinia kockiana Korth. and Its Antibacterial Synergistic Interaction, Appl Biochem Biotechnol, 198(3):1869-1898. doi:10.1007/s12010-025-05497-6. PMID: 41504841.
26.
Viswanathan MB, Jeya Ananthi JD, Sathish Kumar P. (2012), Antimicrobial activity of bioactive compounds and leaf extracts in Jatropha tanjorensis, Fitoterapia, 83(7):1153-9. doi:10.1016/j.fitote.2012.07.007. PMID: 22884742.
27.
Yadav R, Puniya AK, Shukla P. (2016), Probiotic Properties of Lactobacillus plantarum RYPR1 from an Indigenous Fermented Beverage Raabadi, Front Microbiol, 7:1683. doi:10.3389/fmicb.2016.01683. PMID: 27818658.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.